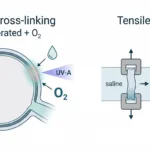
Corneal crosslinking is widely used for progressive keratoconus and other ectatic corneal disorders, where a weakening stroma can drive shape change and vision loss. The procedure is meant to stiffen the cornea by strengthening collagen bonding through a riboflavin plus UV-A photochemical reaction that depends on oxygen. When it works well, corneal crosslinking stabilizes biomechanics enough to slow progression.
Epi-off treatment is well established, but it is not trivial for patients: the epithelium is removed, discomfort is higher, and recovery is longer. That is why epi-on corneal crosslinking remains an active area, with the central question being whether you can keep the epithelium intact and still get a meaningful stiffening response.
In this study by Avedro Inc., the team examined how oxygen concentration, UV-A delivery, and riboflavin formulation affected treatment performance in accelerated epi-on protocols. CellScale contributed to the work through the use of the BioTester, which was used for biomechanical assessment of corneal samples after treatment.
Why corneal crosslinking optimisation matters
The challenge with corneal crosslinking is not simply whether the treatment creates crosslinks. It is whether enough of the key ingredients reach the stroma in the right way to produce a clinically meaningful biomechanical effect. In conventional epi-off procedures, removing the epithelium improves stromal access, but that advantage comes at the cost of greater invasiveness.
With epi-on corneal crosslinking, the intact epithelium can limit stromal delivery of oxygen, riboflavin, and UV-A, all of which are needed to drive the crosslinking reaction. That makes optimisation especially important. If oxygen availability or drug penetration is inadequate, the resulting stiffening effect may be too small to match the performance of epi-off treatment.
This is one reason the study is so useful. It does not treat epi-on CXL as a single protocol. Instead, it asks which combination of oxygen environment, photosensitizer formulation, and light delivery produces the strongest biomechanical response.
For a related read, see our earlier post on the biomechanical impact of corneal crosslinking.
What the researchers tested
The researchers used whole ex vivo porcine eyes held in a custom chamber that allowed acclimatization, treatment, and measurement in parallel. They compared several accelerated corneal crosslinking protocols, focusing especially on epi-on approaches.
The study evaluated:
-
high-irradiance epi-on protocols using riboflavin formulated with benzalkonium chloride
-
those same protocols with and without supplemental oxygen
-
an alternate low-irradiance epi-on protocol using riboflavin formulated with sodium iodide
-
negative and positive control groups for comparison
The main endpoints included stromal oxygen levels, acute corneal flattening, and post-treatment stiffness. That combination made the work especially valuable because it connected treatment chemistry and oxygen transport to actual biomechanical outcome.
Why oxygen mattered in epi-on corneal crosslinking
One of the most important findings was that oxygen support made a major difference. Protocols that included supplemental oxygen produced much higher stromal oxygen levels before treatment and helped maintain a more aerobic state during high-irradiance UV-A exposure. By contrast, under normoxic conditions, stromal oxygen dropped rapidly during treatment.
That matters because oxygen is not just a passive background variable in corneal crosslinking. It is part of the photochemical process that helps drive crosslink formation. If oxygen is depleted too quickly, the treatment effect can become limited, especially in epi-on protocols where transport into the stroma is already constrained by the intact epithelium.
This gives the study a strong translational angle. It suggests that improving oxygen availability may be one of the most practical ways to strengthen the performance of accelerated epi-on treatment.
How the CellScale BioTester was used
CellScale’s role in the study was in the biomechanical evaluation of corneal crosslinking. After treatment, corneal samples were mechanically assessed using the BioTester, which was used as a biaxial extensiometer for corneal tissue testing.
That is an important detail because the value of corneal crosslinking is ultimately biomechanical. The treatment is intended to stiffen the cornea, so direct mechanical testing provides a meaningful way to compare protocols. In this case, BioTester-based testing helped quantify the elastic modulus of cornea after different CXL conditions, showing which treatment combinations produced the strongest stiffening response.

For another example of CellScale work in this area, see our post on cornea testing at the IROC Institute in Zurich, Switzerland.
Mechanical testing of corneal tissue showed stronger stiffening with oxygen support
The biomechanical results showed that not all epi-on protocols performed equally. The combination of supplemental oxygen, a BAC-containing riboflavin formulation, and high-irradiance UV-A produced the largest stiffening response among the epi-on groups. That same protocol also produced the most pronounced acute flattening effect.
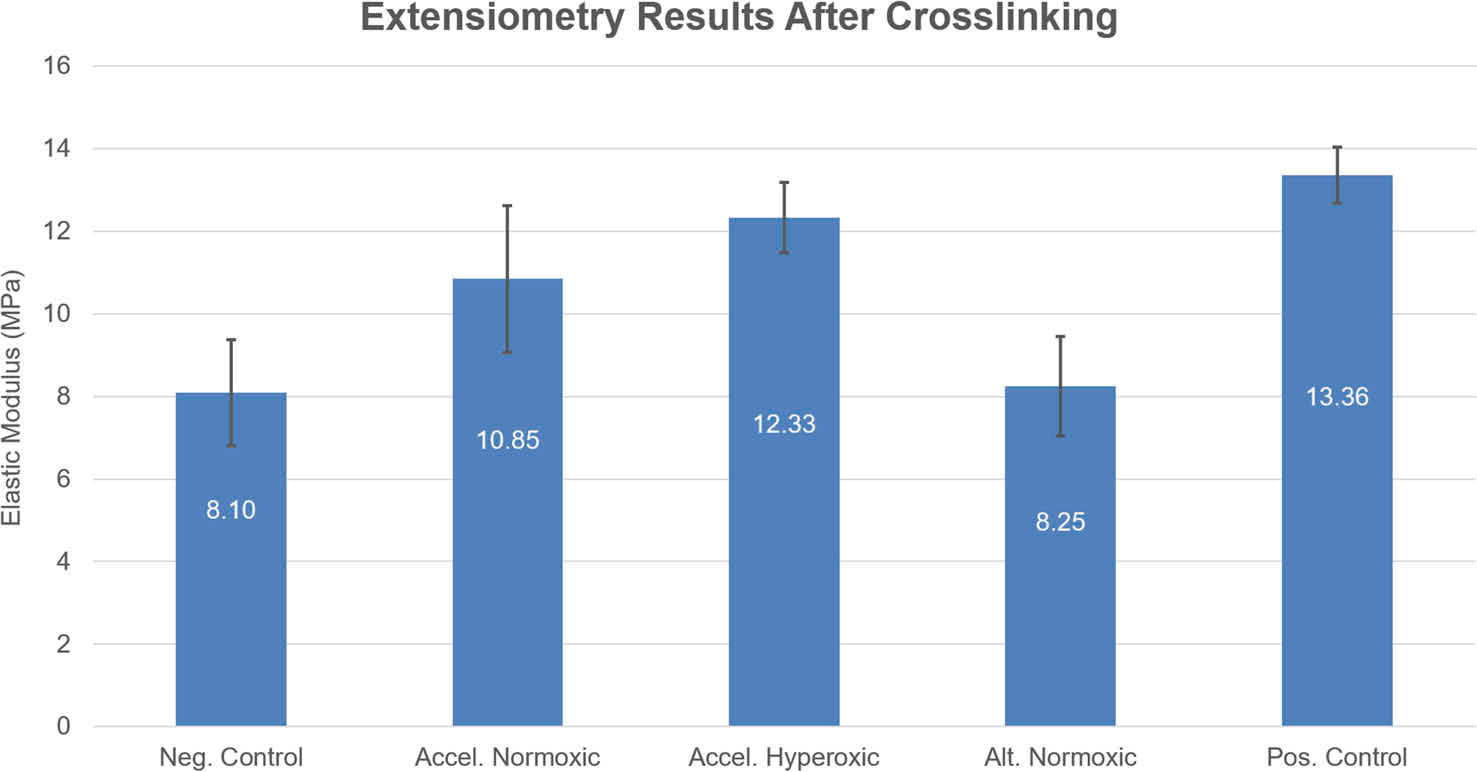
This is where mechanical testing of corneal tissue becomes especially important. It moves the discussion beyond protocol details and into measurable tissue response. Instead of only asking how much oxygen entered the stroma, the study could ask what happened to corneal stiffness after treatment. That is a much more useful question when evaluating protocol performance for keratoconus-related applications.
The finding also strengthens the case for biomechanical evaluation of corneal crosslinking as part of treatment development. If the goal is to stabilize the cornea, then changes in elastic modulus and shape are among the most meaningful outputs.
For a more recent related post, see corneal stiffening to improve transplant outcomes.
Why elastic modulus matters in corneal crosslinking
When discussing corneal crosslinking, elastic modulus is one of the clearest ways to describe whether the tissue became mechanically stronger after treatment. A stiffer cornea is generally better able to resist deformation, which is directly relevant in diseases such as keratoconus where progressive weakening and shape change are central features.
That does not mean elastic modulus tells the whole clinical story, but it is a useful biomechanical marker. In a protocol optimisation study like this one, it helps show whether changes in oxygen supply, drug formulation, and UV-A delivery are producing a meaningful structural effect in the tissue.
For technical readers, this is one of the strongest reasons to include corneal stiffness measurement in the workflow. It anchors protocol comparison in actual tissue mechanics rather than relying only on treatment settings.
What this means for accelerated corneal crosslinking
The main takeaway is that corneal crosslinking performance in epi-on protocols depends on more than irradiance alone. Oxygen availability, riboflavin formulation, and UV-A delivery all worked together to shape the treatment outcome. The strongest biomechanical changes were seen when these variables were optimised together rather than in isolation.
That makes the study especially relevant for anyone interested in accelerated corneal crosslinking and next-generation keratoconus treatment workflows. It shows that epi-on approaches may benefit substantially from oxygen-supported delivery strategies, especially when the goal is to improve stiffness without removing the epithelium.
Final thoughts
This study offers a useful look at how corneal crosslinking protocols can be improved through better control of oxygen environment, photosensitizer formulation, and UV-A delivery. For accelerated epi-on treatment, those variables made a clear difference in stromal oxygen availability, acute corneal flattening, and post-treatment stiffness.
CellScale’s BioTester supported the biomechanical side of that comparison by helping quantify the elastic modulus of treated corneal tissue. That mechanical perspective is important because it shows not just how the protocols differed, but how those differences translated into the property that matters most in crosslinking: corneal stiffening.
Read the publication details here: Optimization strategies for epithelium-on corneal crosslinking